Health & Wellbeing
Expert advice, tips and guidance from medical and healthcare professionals to help you take care of your physical health and mental wellbeing
Explore Health & Wellbeing
Latest
-
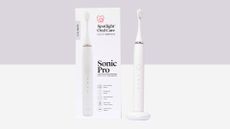
I tried the Spotlight Oral Care Sonic toothbrush - here's why I'll recommend the budget-friendly buy to friends in 2024
The Spotlight Oral Care Sonic toothbrush offers more for your money than some of the big brands, with 30 to 50,000 brush strokes a minute
By Caramel Quin Published
-

These are 32 of the best foods to eat before a workout, whatever your gym goals
Power yourself through exercise with the best foods to eat before a workout
By Lauren Clark Published
-

What does creatine do? The muscle-maintaining supplement explained
Creatine is a great supplement to take if you regularly work out. Here, experts explain what it is, how it works, and the many benefits for women
By Grace Walsh Last updated
-

The 8 best Pilates apps for boosting strength, balance and flexibility in 2024
Our recap of the tried and tested best Pilates apps to download this year, so you can reap the full-body benefits of balance, strength and flexibility
By Lauren Clark Last updated
-

I ran 10km for the first time in 20 years - here's how I trained for it from scratch
Susan Griffin took up learning how to run 10km improve her fitness and get outside her comfort zone this year. Here's how she did it from start to finish line
By Susan Griffin Published
-

These 'super comfortable' Veja running shoes are the perfect combination of supportive and stylish
Health Editor Grace Walsh took the Veja Condor 3 running trainers out for a spin for two weeks - here's how they held up and whether they are worth the price tag
By Grace Walsh Published
-

32 of the best foods to have in the evening
The best foods to have in the evening complement a healthy sleep routine with plenty of vitamins and minerals - but aren't too filling
By Grace Walsh Published
-

I've got the £31 Lululemon lookalike gym leggings everyone is talking about – and, yes, they really are that good
CRZ Yoga Butterluxe leggings are my new go-to gym wear
By Kerrie Hughes Published
-

15 best sex toys to help you reach a mind-blowing orgasm in no time
There's a pick of the best sex toys out there for everyone - here's our selection of the tried, tested, and reviewed favourites for every experience level and budget
By Grace Walsh Last updated
