32 simple but effective tips to help boost your mental health
Although it is always a good idea to speak to a professional if you are struggling, these tips can help to improve your overall mental wellbeing


If you're struggling with your mental health at the moment and want to make some practical changes, there are plenty of simple things you can do to boost your everyday mood.
From confiding in loved ones to learning a new skill, you shouldn't underestimate how simple acts can help you get out of a rut and feeling like yourself again. Most of them won't cost you a penny and can be easily slotted into your usual routine if you're pushed for time.
Although it is always a good idea to speak to a professional when you are particularly struggling with your mental health, implementing just some of these 32 simple tricks can work wonders to make each day feel more positive.
Simple tips to boost your mental wellbeing
While these tips can help cultivate a more positive mindset, they are not professional medical advice. If you are struggling with your mental health, reach out to a GP or a recognised charity, like Mind.
Practice mindfulness

Mindfulness involves focusing solely on the present moment to avoid becoming overwhelmed with other factors in your life. It isn't the easiest thing to put into practice, but it can help to ground yourself in the present moment when you can feel your mind spinning out of control. Allowing yourself to be present in your surroundings rather than thinking about the various stressors in your life can make a real difference to your stress and happiness levels throughout the day.
Why Has Nobody Told Me This Before? by Julie Smith: from £8 at Amazon
No matter what you're dealing with, this book from clinical psychologist Dr Julie Smith shares all the essential coping skills you need to get through life's challenges.
Exercise regularly

Regular exercise is one of the best ways to boost both your physical and mental health. It's important to find a form of exercise that you love and that fits in with your lifestyle to ensure you can stick with it - whether that's cardio training or downloading a workout app to use at home. Even a short walk outside every day could be the thing that makes a difference to you, so don't be afraid to try a few new things.
Drink more water

Everyone knows how important it is to drink enough water, but did you know that it can reduce the risk of depression and anxiety - according to research from the World Journal of Psychiatry? It's an easy thing to overlook in your busy everyday life, but making it into a habit could have even more benefits than you realise.
Sign up to our free daily email for the latest royal and entertainment news, interesting opinion, expert advice on styling and beauty trends, and no-nonsense guides to the health and wellness questions you want answered.
Spend time with animals

Spending time with animals is one of the things that is pretty much guaranteed to improve your mood every time. If you have a pet, make a conscious effort to spend as much time with it as you can. Or, if you don't have any animals of your own, you can spend time with friends' pets or volunteer at a rescue centre or petsit in your spare time.
Start a new hobby

Having a hobby isn't only good for keeping your mind and body active, but it can also help to give you a stronger sense of purpose and fill your days with something that brings you joy. It can be something social like pickleball for beginners or something you can do from the comfort of your own home, such as crafts or reading.
Spend time with loved ones

Although it can be natural to shut people out when you're going through a difficult time, spending time with loved ones is one of the best ways to boost your mental health. Quality time with friends and family can help to take your mind off things, have a good laugh, and provide space for you to offload.
Give to others
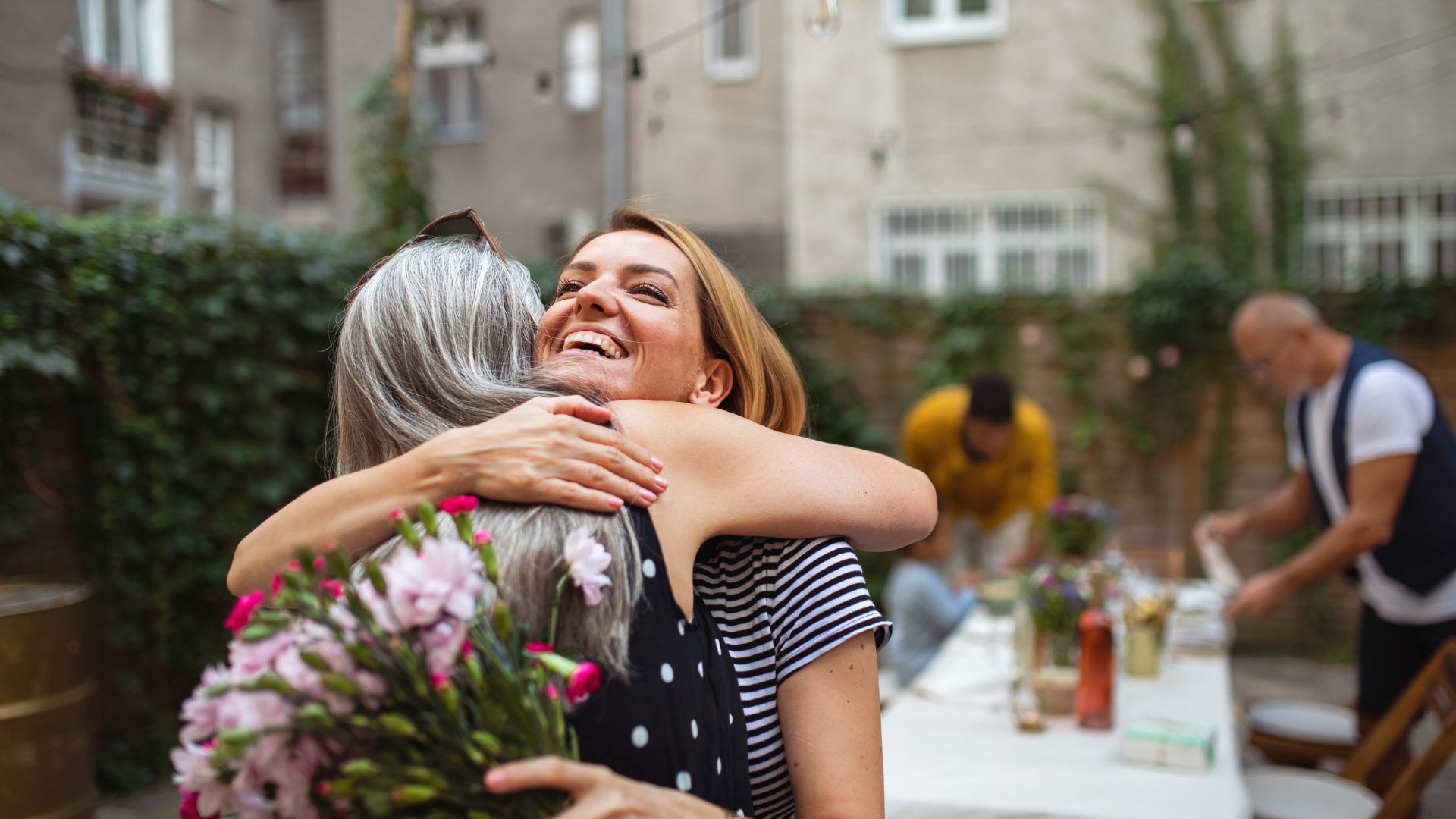
The feeling of giving someone a gift and seeing their happiness is extremely rewarding, so it's a brilliant way to lift both their mood and yours. But giving doesn't just have to be about material things, you can also give your time and support to those who need it and make a real difference.
Take time to relax

Taking time out of your routine to relax and de-stress is extremely important for both physical and mental well-being. If you have the time, a proper pampering session will always make you feel better. However, you can also relax with a short nap, shower, reading a few pages of a book, or sitting outside when you get the chance. No matter how you like to relax, it should be an essential part of your day if you want to feel your best.
Spend time in nature

Spending time in nature is one of the top recommendations for boosting your mental health. From wild swimming and hiking to just strolling around your local green space, any time spent outdoors will help to clear your mind and enrich the soul when you need it.
Eat well

Eating a healthy, balanced diet will keep both your body and mind feeling good. Giving yourself the nutrients you need to function well will ensure you feel your best day-to-day, and improve your energy levels so you can get the most out of your day. From high-protein foods to keep you full for longer to delicious fruits and veggies, there are countless ways to improve your diet for noticeable changes.
Try to improve your sleep

The importance of good sleep cannot be overstated. If you're not sleeping properly, your brain cannot function and your mental health will likely become worse. There are plenty of ways to improve your sleep, from meditation and improving your sleep setup to seeking medical advice when necessary.
Join a new class or group

Starting something new can be daunting, but joining a class or group to learn or improve on a skill can be incredibly fulfilling and give you more purpose in your week. Not only will you feel a sense of accomplishment, but you could also make some great new friends.
Do something creative

Creative pursuits like art and music can not only help you to relax and disconnect, but can also enrich your life. Something as simple as colouring has been known to help people switch off and take time away from screens or distractions, even if only for a short while.
Don't be afraid to ask for support

Managing stress is much easier said than done, and most of the time it probably feels like it's out of your control. However, there are small things you can do to keep your stress levels at bay. Talking to someone about how you're feeling and allowing others to help is the first crucial step. With stress in the workplace especially, it is always a good idea to ask for support where you need it.
Bring nature inside

It isn't always possible to spend time outside in our busy routines, so bringing aspects of nature indoors is a great way to brighten your day. Having fresh flowers or plants inside is a small detail but one that can help to put a smile on your face.
Talk to someone you trust

Having someone you trust to confide in is extremely important for your mental well-being. A problem shared is a problem halved, and having somebody to speak to can work wonders to change your perspective or to help you feel less alone in whatever you are going through.
Volunteer

Volunteering for a cause you feel strongly about is a brilliant way to feel good and see how your actions can directly improve the lives of others. Whether it's a one-off or a regular volunteering gig, it is bound to give you a sense of pride and accomplishment that can improve your mental wellbeing.
Establish a routine

Establishing a daily routine can make a huge difference to your everyday mental state. A lack of routine can often make us feel purposeless or unproductive, so having even a few things that you stick to every day is a good idea if you want to feel more fulfilled.
Reduce screen time

It's no secret that reducing screen time can improve your mental health. Not only does it take you away from the often upsetting or stressful news that we can be exposed to online, but it also encourages you to spend more time doing more enriching things, such as spending time outside or focussing on your hobbies.
Try journaling

Journaling can take a little while to get into, but it is a very valuable tool for letting out your emotions in a safe and private space. It can also help you to identify your main worries and concerns, regulate your emotions, and process information healthily.
Plan something to look forward to

Having something in your life to look forward to is a brilliant way to remain optimistic. It can be something big like a trip abroad, or something small like eating your favourite meal at the weekend or a coffee date with friends. Try to have something every month that you can look forward to to give you something to focus on and keep you feeling happy in your low moments.
Eat your favourite food

Eating your favourite food is an easy way to lift your mood. Sometimes something as simple as this can make you feel much better on a rubbish day, especially if it isn't something you have regularly. Of course, small treats won't solve any serious issues - but they will brighten your day.
Get as much sunshine as possible

Vitamin D from the sun not only keeps your immune system functioning healthily, but it can also reduce symptoms of depression. Depending on where you live it can be tricky to get a lot of sun, but when it does show itself, it's always a good idea to get outside and take it in.
Have a morning ritual

Starting your day in the right way can set your mood on track, so it can be useful to have some sort of ritual that gets you up. It could be making the bed or showering as soon as you wake up, but no matter what you choose, it can be a useful tool to begin your day on a positive and productive note.
Take vitamins and supplements

If you struggle to get your vitamins naturally, supplements can work wonders to give your body what it needs to feel happy and healthy. From Vitamin D supplements to multivitamins, taking what you need daily can improve your physical and mental health.
Be kind to others

Being kind to others will always make you feel good too. From small acts of kindness to large gestures, you never know how much difference you could be making to someone's life by treating them well, and you will likely find that you are met with kindness in return that will boost your mood significantly.
Meditate

Meditation can help to reduce feelings of stress and help you to live in the present. As a way to step outside of the current challenges you are facing, it offers a form of escapism that can be invaluable when you are in a tough mental space.
Make your home a welcoming and safe space

Being in a safe and welcoming space can help you feel better when you're in a rut. Simply redecorating or investing in some interior accessories to transform your space can often be the breath of fresh air you need, and can help you to feel relaxed and calm.
Treat yourself

Although it's wise to be mindful of your spending, sometimes splurging on a treat or two for yourself can really pick you up. It doesn't have to be anything expensive - it could just be a nice cup of coffee or a new accessory - but giving yourself a gift when you deserve it has the power to lift your mood.
Practice gratitude

Despite your struggles, it is important to be grateful for the many good things in your life. The presence of good things doesn't eliminate the bad, but often reflecting on the positives can help you to recognise the great parts of your life or notice your many achievements that past you would be proud of.
Listen to your favourite music

Nothing can change your mood quite like listening to your favourite songs. No matter where you are or what you're doing, putting your headphones on and blasting music you love is bound to improve how you're feeling for even a short while.
Remember how you're feeling won't last

When times are especially difficult, it's important to remember that no bad feeling lasts forever. You have overcome plenty of challenges before and you can do it again.

Amelia joined woman&home in 2022 after graduating with an MA in Magazine Journalism from City University and she is now a senior fashion and beauty writer. She began building her career as a lifestyle journalist after completing a fashion journalism course at the Condé Nast College of Fashion & Design in 2019, writing for a variety of titles including OK!, New!, and Notion on topics such as sustainable fashion and entertainment.

